Alright, let’s get real about that unwelcome guest: a vulvovaginal yeast infection. You know it as candidiasis or plain old thrush. It’s when that sneaky Candida fungus, which usually just chills out in small numbers, decides to throw a full-blown party in your vagina. And what’s the result? Oh, just intense itching, burning, that lovely thick discharge, and general discomfort that makes you want to crawl out of your skin. Most of us ladies will deal with at least one in our lifetime, and usually, a quick antifungal cream or a dose of fluconazole sends it packing. But for a frustrating 8-10% of women? Those damn infections just keep coming back – we’re talking four or more episodes a year, officially called recurrent vulvovaginal candidiasis (RVVC). Talk about a nightmare that seriously messes with your life! But here’s the hook, the silver lining: don’t despair! Most of these stubborn cases can totally be tamed with the right diagnosis, proper treatment, and smart prevention. You’ve got this!
Why That Damn Yeast Infection Keeps Showing Up Again (The Real Talk)
Listen up: it’s rarely just about your body being “resistant” to treatment. Oh no, it’s usually a whole cocktail of factors throwing your vaginal balance completely out of whack. Get ready to uncover the usual suspects behind those stubborn recurrent yeast infections:
- Hormonal Changes: Your hormones are like a roller coaster, right? Estrogen swings – hello, pregnancy, birth control, HRT, menopause – can basically roll out the red carpet for Candida to thrive.
- Antibiotic Use: Ah, antibiotics. They’re great for what they’re prescribed for, but they’re also notorious for wiping out the good bacteria (your lactobacilli squad) that normally keep yeast in check. It’s like leaving the bouncer off duty! A super common trigger for a comeback.
- Uncontrolled Diabetes/High Blood Sugar: Here’s a no-brainer: yeast absolutely LOVES sugar. If your blood sugar levels are all over the place because of poorly managed diabetes, you’re basically serving up a buffet for Candida.
- Weakened Immune System: When your immune system is down – thanks to stress, illness, or certain meds (like steroids or chemo) – it’s less able to fight off invaders. Guess who takes advantage? Yep, yeast.
- Lifestyle Factors: This is where you might be unknowingly shooting yourself in the foot. Think tight, non-breathable undies, constant moisture, douching, or those “fragrant” products. They all mess with your natural pH and flora, creating a prime breeding ground.
- Non-Albicans Candida or Misdiagnosis: Sometimes, it’s not the usual suspect. Less common species of Candida (like C. glabrata) can be super stubborn and laugh in the face of standard treatments. Or, maybe it wasn’t even a yeast infection to begin with – symptoms can totally mimic bacterial vaginosis (BV) or other issues. Get it checked!
- Sexual Activity (Rarely Direct Transmission): While it’s not typically “passed” like an STI, sexual activity can sometimes irritate things down there or even reintroduce yeast. But let’s be clear, it’s not the primary villain in most recurring cases.
| Risk Factor | How It Contributes | Prevention Tip (Your Action Plan!) |
|---|---|---|
| Antibiotics | Wipes out your good, protective bacteria. | Pop those probiotics during and after your course – seriously, they’re your allies! |
| Hormonal Shifts | Pumps up the glycogen, which is basically gourmet food for yeast. | Chat with your doctor about your options. Don’t just suffer in silence! |
| Diabetes | Sky-high sugar levels? You’re practically inviting yeast to a feast. | Get that blood sugar under tight control. It’s non-negotiable for prevention. |
| Tight Clothing/Moisture | Creates a sauna-like environment – perfect for yeast to party. | Switch to breathable cotton undies; make sure you’re bone-dry down there. No dampness allowed! |
| Douching/Scented Products | Completely throws off your natural pH balance – a recipe for disaster. | Ditch ’em! Stick to plain water for cleaning. Your vagina is self-cleaning, trust it. |
Is It a Yeast Infection? Here’s What to Look For (Don’t Ignore These!)
You’re probably experiencing intense itching and burning in your vulva and vagina – it’s usually impossible to ignore.
That tell-tale thick, white discharge, often described as looking like cottage cheese. (And thankfully, usually odorless, unlike some other issues.)
You might notice redness and swelling, making everything feel even more irritated.
Pain during sex or when you pee? Yep, that’s another common, unwelcome symptom.
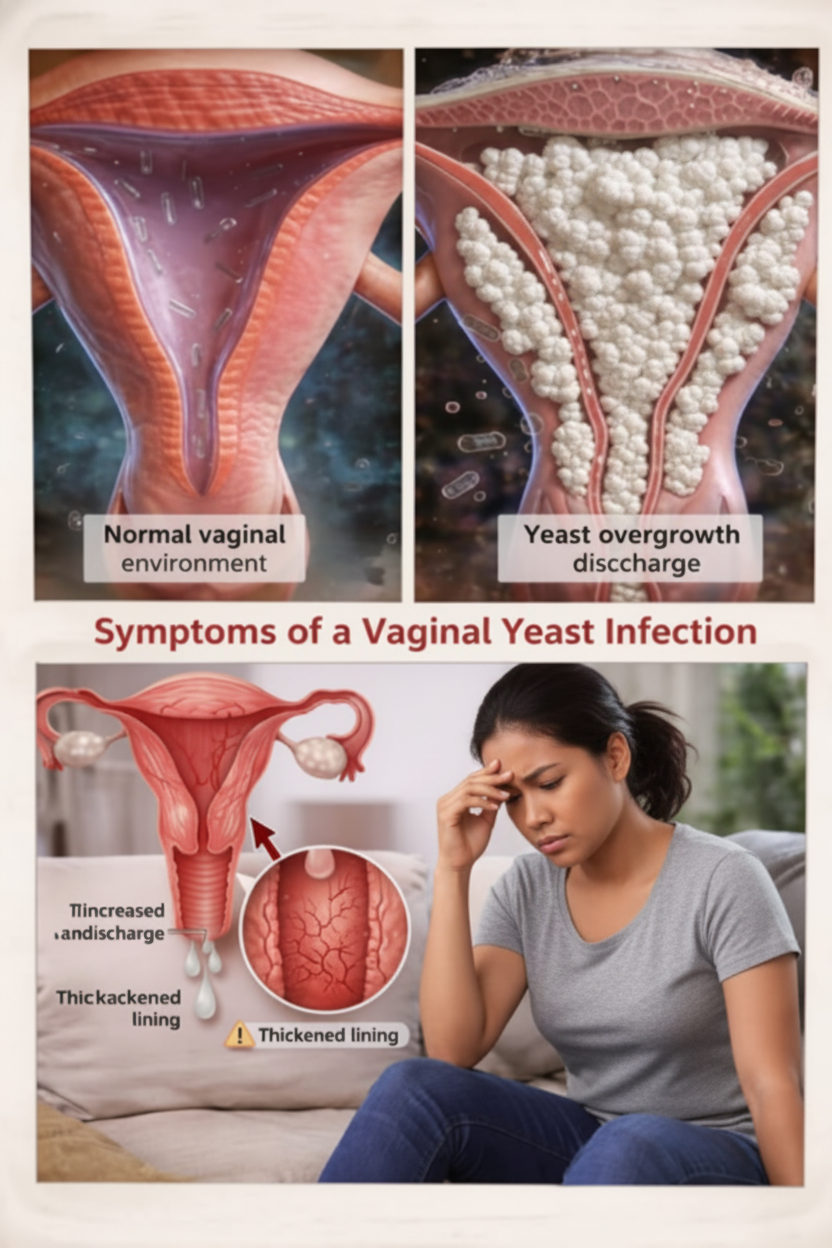
If these symptoms keep crashing your party, especially if they’re recurring, don’t just guess! Get tested. A proper culture will identify exactly what species of yeast is causing havoc, so your doctor can hit it with the right, targeted treatment. No more shooting in the dark!
Finally Kicking RVVC to the Curb: Your Treatment Playbook
Straight from the experts – the CDC and Mayo Clinic – here’s the lowdown on how to tackle those stubborn recurrent yeast infections:
- Initial Attack Plan: Don’t mess around with short courses anymore. Your doctor will likely prescribe a longer, more aggressive antifungal course – think 7-14 days of topical cream or oral fluconazole. We’re going for a knockout!
- Maintenance Mode: Once you’ve got it under control, the goal is to keep it that way. This often means a weekly dose of fluconazole for a solid 6 months. This strategy is a game-changer, slashing recurrence rates by about 90%!
- New Heavy Hitters: Good news on the horizon! Keep an eye out for newer options like Oteseconazole (FDA-approved in 2022 specifically for RVVC) and ibrexafungerp. These are designed to tackle the toughest cases.
- Probiotics (Proceed with Caution): While oral or vaginal lactobacilli probiotics sound promising for prevention, the research is a bit mixed. Some swear by them, others don’t see a huge difference. Talk to your doc if you’re considering them.
Smart Moves: Prevention Strategies That ACTUALLY Work!
- Ditch the synthetics! Always opt for breathable cotton underwear. Let things breathe down there.
- Seriously, stop douching and steer clear of scented pads or tampons. They just throw your natural balance into chaos.
- Always, *always* wipe front-to-back after using the toilet. It’s basic hygiene, but crucial for keeping unwanted bacteria away.
- Got sweaty from a workout or a swim? Change out of those wet clothes ASAP. Moisture is yeast’s best friend.
- Get a handle on your blood sugar (if applicable) and find ways to manage stress. Both can seriously impact your body’s ability to fight off infections.
- If you’re constantly on antibiotics, chat with your doctor about whether probiotics could be a smart addition to your routine.
When It’s Time to Stop Messing Around and Call the Doctor (Don’t Wait!)
If those symptoms are still hanging around after you’ve tried over-the-counter treatments, it’s a clear sign you need professional help.
Are you hitting 4 or more episodes of infection per year? That’s a red flag for recurrent vulvovaginal candidiasis, and it definitely warrants a doctor’s visit.
<