Sudden Eye Floaters, Flashes, or Shadows: Your Urgent Guide to Vision Care
Experiencing small specks or shapes drifting through your field of vision can be disconcerting. These “eye floaters” often become a source of significant concern when they appear abruptly, increase rapidly in number, or are accompanied by sudden flashes of light or a dark, curtain-like obstruction across your sight. While it’s common to dismiss such symptoms as mere fatigue or stress, they can, in fact, signal a serious underlying eye condition requiring immediate evaluation. The crucial takeaway is that understanding the warning signs and knowing how to respond within the critical 24-hour window can be pivotal for preserving your vision. Pay close attention, as we reveal a frequently missed symptom later in this essential guide.
Understanding Eye Floaters: What Are These Visual Disturbances?
Known medically as vitreous floaters, these are small, often translucent specks or shapes that appear to move across your line of sight. Their appearance can vary widely, often described as:
- Minute dark or grayish dots
- Delicate, cobweb-like filaments
- Wiggly, transparent lines
- Subtle, shadowy patches
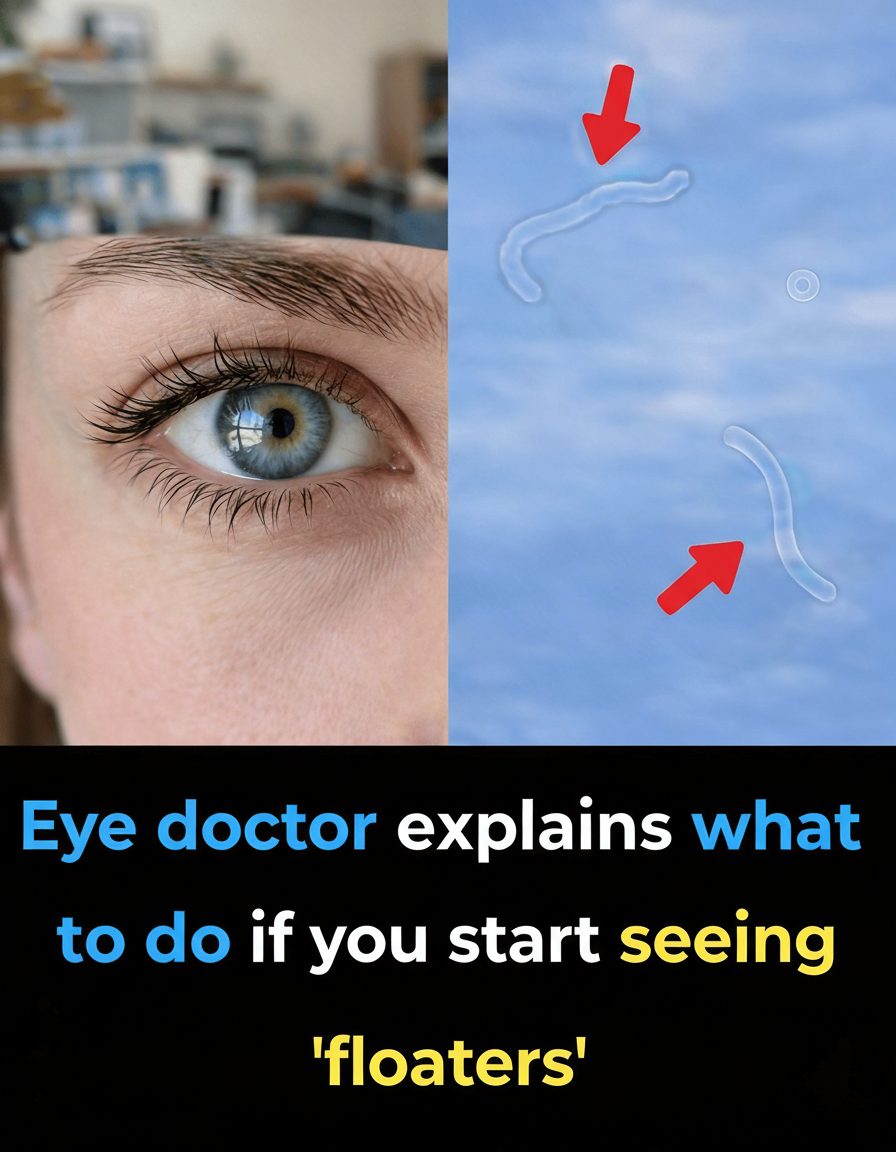
These phenomena typically follow your eye movements and become particularly prominent when gazing at a bright, uniform background, such as a clear blue sky or a plain white wall. The internal structure of your eye contains a clear, jelly-like substance called the vitreous humor. As we age, this gel can naturally undergo changes, leading to slight shrinkage or the formation of tiny clumps. These irregularities cast minute shadows onto the retina, the light-sensitive tissue located at the rear of your eye. It is these shadows that you perceive as floaters.
For the most part, eye floaters are benign and tend to diminish in noticeability over time as your brain learns to filter them out. Indeed, many eye care professionals observe the remarkable ability of the brain to adapt to and ignore consistent floaters. However, this isn’t universally true, and certain changes warrant immediate attention.
When Eye Floaters Demand Urgent Professional Attention
While many floaters are harmless, a sudden alteration in their presentation can be a critical indicator of a more severe ocular condition, such as a potential retinal tear or even a retinal detachment. Leading health organizations, including University of Utah Health, strongly advise seeking immediate ophthalmological care within 24 hours if you experience any of the following:
- A dramatic and sudden surge in the number of new dark spots
- Persistent flashes of light in the affected eye, particularly noticeable in low-light conditions
- The appearance of a shadow, a gray curtain, or a distinct dark area obstructing any part of your visual field
- Any rapid or significant changes in the characteristics or quantity of existing floaters
These alarming symptoms suggest that the delicate retina might be under undue traction or has sustained a tear. Retinal complications are inherently time-sensitive; prompt diagnosis and intervention are paramount to avert further vision loss and preserve ocular health. Even when symptoms appear minor, the speed of response can profoundly impact the outcome.
Emergency Intervention vs. Scheduled Monitoring: Knowing the Difference
To ensure clarity, let’s delineate when immediate action is required versus when a timely appointment suffices. Seek emergency eye care without delay if you encounter:
- The abrupt onset of many new floaters
- Sudden, recurring flashes of light within a single eye
- A distinct shadow or veil obscuring a portion of your vision
In such scenarios, procrastination is not an option. Contact an eye care professional or emergency medical services within 24 hours.
Conversely, you may monitor and schedule a non-urgent appointment if you observe:
- Just one or two isolated, small floaters
- An absence of associated light flashes
- No visual obstruction or shadow in your field of vision
- No noticeable increase or change in the floaters over a short period
For these less critical situations, arrange a consultation with an ophthalmologist within a few days. The overarching principle remains: if uncertainty persists, always opt for a professional examination. It is always preferable to conclusively rule out a serious condition than to assume benignity and potentially risk your vision.
What to Expect During Your Eye Examination for Floaters
Upon visiting an ophthalmologist concerning floaters, the initial step typically involves administering dilating eye drops. These drops temporarily enlarge your pupils, allowing the specialist an unobstructed view of the intricate structures at the back of your eye. The ophthalmologist will then meticulously examine your retina and vitreous humor, searching for any indicators of tears, hemorrhage, or detachment. While the dilating drops may induce temporary blurred near vision and increased light sensitivity for several hours post-examination, the procedure itself is generally comfortable and painless.
A frequent cause of sudden floaters, particularly in older adults, is a condition known as posterior vitreous detachment (PVD). This common, age-related change occurs when the vitreous gel naturally separates from the retina. Peer-reviewed research in ophthalmology confirms that PVD is prevalent in individuals over 50 and typically resolves without leading to chronic vision problems. Nevertheless, a thorough evaluation is indispensable to confirm PVD and, more importantly, to rule out any more severe underlying conditions that could threaten your eyesight.
Understanding the Phenomenon of Light Flashes in Your Vision
Flashes of light, medically termed photopsia, arise when the vitreous gel exerts a slight tugging or rubbing sensation against the retina. The retina, being the light-sensitive tissue, misinterprets this mechanical stimulation as actual light, even in the absence of external light sources. These flashes can manifest in various forms, such as:
- Fleeting streaks resembling lightning
- Sudden, bright bursts akin to a camera flash, often in peripheral vision
- Subtle, flickering lights, particularly noticeable in dimly lit environments
While sporadic, brief flashes that quickly subside might be benign, persistent or recurrent flashes, especially when combined with the sudden appearance of new floaters, necessitate an immediate and thorough ophthalmic assessment. This combination of symptoms can be a critical warning sign.
Your Immediate Action Plan Upon Noticing Floaters
Should you suddenly become aware of floaters, follow these practical steps:
- Remain Calm, but Observe Diligently: Take note of the exact timing of their onset, their approximate number, whether they appear to be multiplying, and if they are accompanied by any flashes of light or shadows. Jotting down these details can be incredibly helpful for your eye care specialist.
- Assess Each Eye Individually: Gently cover one eye, then the other. This simple test helps determine if the symptoms are confined to a single eye or present in both, providing crucial diagnostic information.
- Refrain from Self-Diagnosis: While the internet offers a wealth of information, online forums and general articles cannot substitute for professional medical advice. Each individual case of eye floaters is unique and requires a personalized assessment.
- Seek Care According to Symptom Severity: Refer back to the “Emergency Intervention vs. Scheduled Monitoring” section provided earlier in this guide to determine the appropriate level and urgency of care required.
Do Eye Floaters Disappear Spontaneously?
Often, yes, many eye floaters do become less noticeable over time. While the floaters themselves typically don’t vanish entirely, the brain’s remarkable neuro-adaptation process learns to filter them out, making them much less distracting. However, some floaters, particularly larger or denser ones, may persist and continue to be a nuisance. Regardless of whether they fade, the initial appearance of new or significantly changed floaters, especially with flashes or shadows, always warrants a professional eye examination to rule out any serious underlying conditions. Never assume they will simply disappear if warning signs are present.