Cervical cancer originates in the cells of the cervix, which is the lower segment of the uterus connecting to the vagina. Leading health organizations, including the American Cancer Society and Mayo Clinic, highlight that the vast majority of cases are associated with persistent infection by high-risk strains of human papillomavirus (HPV). HPV is a widespread virus primarily transmitted through sexual contact. The critical takeaway is that when this cancer is identified at an early stage, often through consistent screening, the prognosis and treatment success rates improve dramatically.
However, many individuals unfortunately overlook initial indicators because early symptoms can easily be mistaken for other prevalent conditions, such as minor infections or typical menstrual fluctuations. Medical studies underscore the importance of self-awareness—attentively monitoring your body and promptly consulting a healthcare professional about any unusual changes can facilitate earlier diagnosis. Crucially, even without noticeable symptoms, routine medical examinations remain the most effective strategy for detection, as cervical cancer in its nascent stages frequently presents without any overt signs.
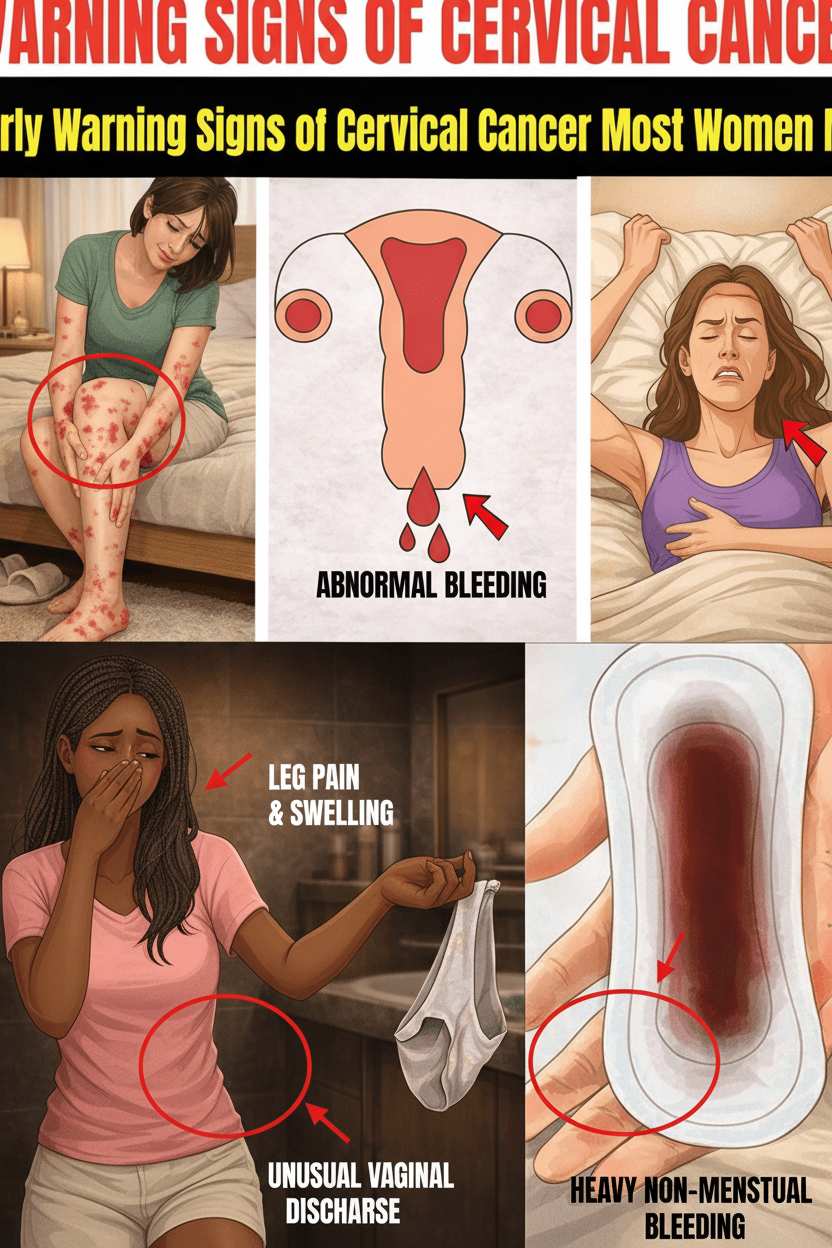
Key Warning Signs to Watch For
Recognizing the potential indicators of cervical cancer is vital. While these symptoms can often be attributed to various non-cancerous conditions, reputable health organizations such as the Mayo Clinic, CDC, and American Cancer Society consistently emphasize their importance. If any of these signs persist, immediate medical consultation is strongly advised.
Abnormal Vaginal Bleeding
This symptom frequently ranks as one of the most commonly reported indicators. It can manifest as unexpected spotting or bleeding between menstrual cycles, following sexual activity, or after menopause. Additionally, menstrual periods that become noticeably heavier or extend beyond their typical duration also warrant medical attention. Esteemed organizations like the NHS and Cancer Research UK unequivocally state that any form of unexplained vaginal bleeding is abnormal and necessitates prompt evaluation by a healthcare provider.
Unusual Vaginal Discharge
Any alteration in the color, consistency, or odor of vaginal discharge should be a cause for concern. This could include discharge that appears unusually watery, bloody, pinkish, brownish, or emits a strong, unpleasant smell. If you experience discharge that is heavier than your usual or occurs outside your normal menstrual cycle, it’s advisable to monitor it and seek professional medical guidance.
Pain During or After Intercourse
Experiencing discomfort or pain during or following sexual intercourse, medically termed dyspareunia, is another potential sign documented by institutions such as MD Anderson Cancer Center. This sensation might be described as sharp or aching and may persist over time.
Persistent Pelvic or Lower Back Pain
Chronic pain localized in the pelvic region, lower back, or abdomen that is not associated with your menstrual period or a clear injury could indicate more advanced cellular changes. This discomfort might present as a feeling of pressure or a dull, persistent ache.
Other Potential Indicators (Often Later Stage)
While less common, certain medical reviews also mention other symptoms that typically emerge in later stages. These can include unexplained leg swelling, persistent fatigue without a clear cause, or alterations in bowel or bladder habits due to pressure from growing tissue.
To help differentiate between common occurrences and potentially concerning signs, consider this quick comparison:
- Normal menstrual spotting: Characterized by light, infrequent bleeding that is typically linked to your menstrual cycle.
- Concerning bleeding: Marked by persistence, occurrence outside your regular cycle, after sexual activity, or post-menopause.
- Typical discharge: Generally clear or white, with a mild odor, and fluctuates naturally throughout your cycle.
- Unusual discharge: Distinguished by a foul smell, a bloody tint, or a constant presence.
It is paramount to seek medical advice if any of these symptoms persist for more than a couple of weeks. Timely consultation with a healthcare professional is crucial.
Why Early Warning Signs Are Often Overlooked
In the rush of daily life, it’s common to dismiss bodily changes, attributing them to factors such as stress, natural aging, or minor, transient infections. Furthermore, many individuals experience embarrassment or discomfort when discussing intimate vaginal health concerns, despite healthcare providers being accustomed to addressing such issues routinely. The reality is that nascent cervical changes progress gradually and frequently without causing any pain, underscoring the immense value of regular screening tools like Pap smears and HPV tests.
Notably, recent guidelines from the American Cancer Society (with updates as recent as 2025) have introduced more accessible screening methods, including self-collection options for HPV testing in specific scenarios, aiming to broaden participation in vital early detection efforts.
Empowering Yourself: Proactive Steps for Cervical Health
Take charge of your cervical health by adopting these evidence-backed practices recommended by health professionals:
Schedule Regular Screenings
- Adhere to current screening guidelines: Generally, women aged 21-29 are advised to undergo a Pap test every three years. For those aged 30-65, a combination of Pap and HPV testing every five years, or as otherwise recommended by their physician, is often suggested.
- Engage in a discussion with your doctor regarding your individual risk factors and the most appropriate screening schedule for you.
Monitor and Track Your Symptoms
- Maintain a simple record of any changes in your menstrual cycle, discharge, bleeding patterns, or pain.
- Document specific dates, the intensity of symptoms, and any potential triggers. This detailed information will be invaluable when consulting with your healthcare provider.
Consider HPV Vaccination if Eligible
- The HPV vaccine offers robust protection against the high-risk strains of the virus that are responsible for most cervical cancers.
- While most effective when administered before exposure to HPV, the vaccine can still provide significant benefits for many adults. Consult your doctor to determine your eligibility and discuss the advantages.
Adopt Healthy Lifestyle Practices
- Prioritize safe sexual practices by consistently using barrier protection during intimacy.
- Avoid smoking, as it is a known risk factor for cervical cancer.
- Support your overall well-being and immune system through a balanced diet and regular physical activity.
Promptly Seek Medical Advice
- If you experience any persistent or concerning symptoms that feel “off,” do not hesitate to contact your gynecologist or primary care provider immediately.
- Early discussions can either offer reassurance or facilitate prompt diagnosis and timely medical intervention, which are critical for optimal outcomes.
Incorporating these preventive measures into your routine requires minimal effort but contributes significantly to your long-term cervical health and protection.
Prevention and Lifestyle Support for Optimal Cervical Health
While regular screenings are paramount, a holistic approach to cervical health also encompasses various lifestyle choices. Scientific research consistently demonstrates that certain habits can significantly support your overall well-being and potentially reduce your risk. These include maintaining a healthy immune system through balanced nutrition, engaging in regular physical activity, and making informed decisions about sexual health. By integrating these practices, you actively contribute to a stronger defense against cervical cancer and promote enduring health.