Uterine fibroids, often referred to as leiomyomas, are a remarkably common concern, impacting a significant majority—up to 80%—of women before menopause. Despite increasing awareness and advancements in women’s health, many still grapple with the perplexing question of why these non-cancerous growths continue to develop. These benign uterine tumors can manifest a range of challenging symptoms, from debilitating heavy menstrual bleeding and persistent pelvic pressure to chronic fatigue, profoundly disrupting daily routines and causing considerable anxiety. It’s particularly frustrating when seemingly diligent lifestyle adjustments don’t appear to halt their progression, leaving many feeling a lack of control.
While the precise origins of fibroids remain multifaceted, extensive research highlights that a comprehensive understanding of their key influences, coupled with the adoption of supportive health habits, can significantly impact risk management and overall well-being. This article delves into the primary reasons why these uterine growths remain prevalent and outlines actionable strategies that women can embrace to foster better health. We’ll also uncover a crucial, yet frequently underestimated, connection that often goes unnoticed until symptoms become more pronounced.
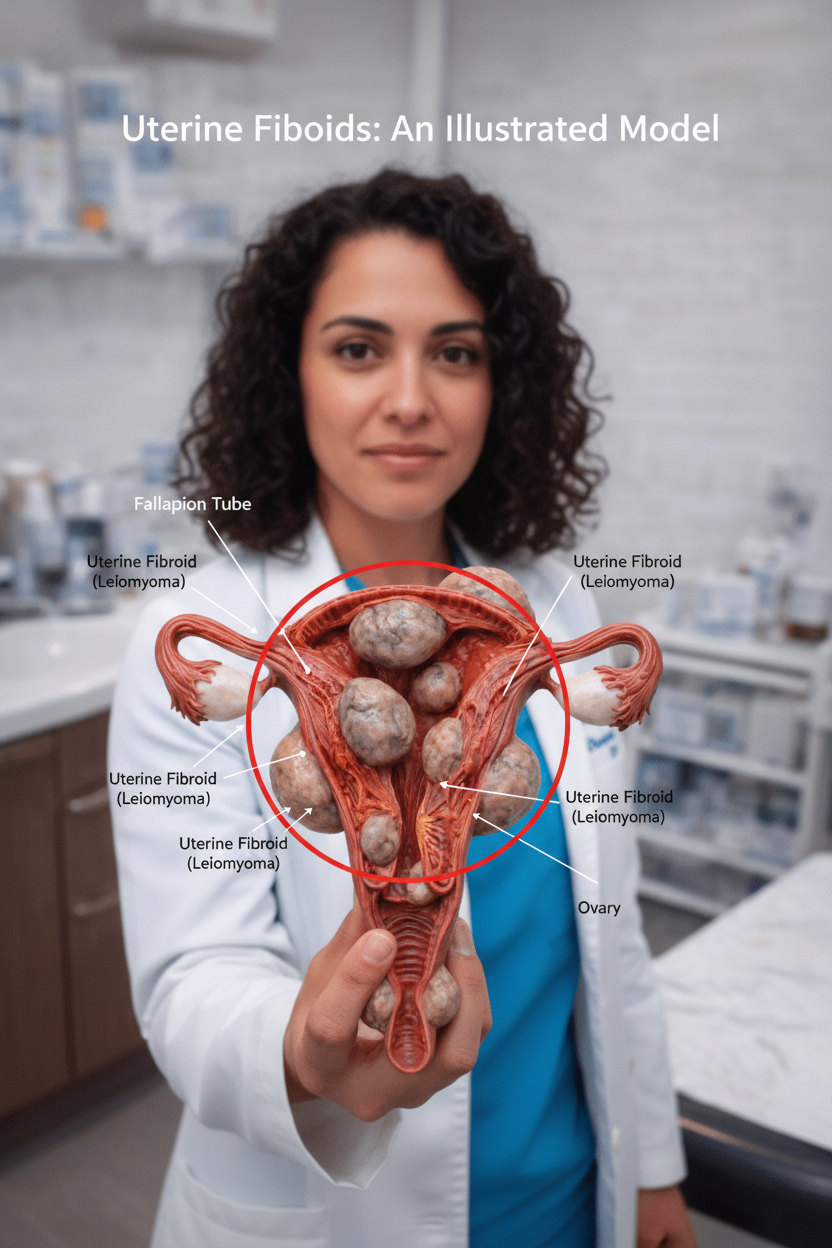
What Exactly Are Uterine Fibroids?
Uterine fibroids, medically known as leiomyomas, are prevalent benign growths composed of smooth muscle cells and fibrous connective tissue. They typically form within the wall of the uterus, or sometimes protrude from its outer surface or into the uterine cavity. Their size can vary dramatically, from microscopic “seedlings” that are undetectable to the naked eye, to substantial masses capable of significantly altering the uterus’s shape and size. These growths predominantly emerge during a woman’s reproductive years, a period characterized by elevated hormone levels. It is a common observation that fibroids tend to regress and often shrink following menopause, coinciding with a natural decline in estrogen and progesterone production.
Crucially, uterine fibroids are nearly always non-cancerous and do not elevate a woman’s risk of developing uterine cancer. Nevertheless, their impact on individual women can differ immensely; some may carry fibroids without experiencing any noticeable symptoms, while others endure considerable discomfort and disruption to their quality of life.
Why Do Fibroids Still Develop in So Many Women?
While the precise etiology of uterine fibroids remains a subject of ongoing scientific inquiry, current understanding suggests their development stems from a complex interplay of several factors. Hormones, particularly estrogen and progesterone, are unequivocally central to their growth. These hormones are essential for the cyclical thickening of the uterine lining, and interestingly, fibroid cells exhibit a higher concentration of receptors for both estrogen and progesterone compared to normal uterine tissue, making them highly responsive to hormonal fluctuations. Beyond hormonal influences, genetic alterations within the uterine muscle cells themselves can predispose them to abnormal and rapid proliferation, especially when exposed to these growth-promoting hormones.
Furthermore, an accumulation of environmental exposures and various lifestyle elements over time are believed to contribute to fibroid development. The prevalence of fibroids in a large segment of the female population can be attributed to the synergistic effect of these diverse influences converging during a woman’s prime reproductive years. Key reasons for their continued commonality include:
- Sustained Hormonal Exposure: Extended periods of elevated estrogen and progesterone levels provide a fertile environment for fibroid growth and expansion.
- Genetic Susceptibility: A woman’s genetic makeup, specifically certain inherited gene variations, can significantly heighten her predisposition to developing fibroids.
- Additional Contributing Factors: Emerging research points to other elements, such as chronic inflammation, oxidative stress, and even early-life exposures, as potential initiators or accelerators of fibroid formation.
Key Risk Factors That Increase the Likelihood
A variety of factors can elevate a woman’s predisposition to developing uterine fibroids. Esteemed medical organizations, including the Mayo Clinic and various NIH studies, have identified these influences. It’s important to distinguish between risk factors that are unchangeable and those that can be influenced by personal choices.
Non-Modifiable Risk Factors: These are elements beyond an individual’s control:
- Age: The incidence of fibroids significantly increases in women during their 30s, 40s, and early 50s, often declining after menopause.
- Race and Ethnicity: Research consistently shows that Black women have a notably higher prevalence of fibroids, often experiencing them at an earlier age and with more severe symptoms, compared to women of other racial backgrounds.
- Family History: A genetic component is evident; if your mother or sister has had fibroids, your own risk is substantially elevated.
Modifiable Risk Factors: These are lifestyle and environmental factors that research frequently associates with an increased fibroid risk:
- Obesity or Higher Body Mass Index (BMI): Adipose (fat) tissue is metabolically active and can produce excess estrogen, which fuels fibroid growth.
- Dietary Habits: A diet rich in red meat and processed foods, but low in fresh fruits and vegetables, has been linked to a higher risk.
- Vitamin D Deficiency: Insufficient levels of Vitamin D are increasingly recognized as a potential contributor to fibroid development.
- Early Onset of Menstruation: Beginning menstruation at a young age (typically before 10 years old) may expose the uterus to estrogen for a longer duration over a lifetime.
- Never Having Been Pregnant: Women who have never carried a pregnancy to term appear to have a somewhat higher risk of developing fibroids.
What often comes as a surprise to many is how subtly, yet profoundly, routine daily habits and environmental exposures can incrementally impact hormonal equilibrium and systemic inflammation over years, ultimately contributing to fibroid risk despite general health awareness.
Lifestyle Habits That May Help Support Uterine Health
While no single strategy can definitively guarantee the prevention of uterine fibroids, a substantial body of evidence indicates that adopting specific lifestyle habits can play a crucial role in mitigating risk or effectively managing existing symptoms. The focus should be on implementing sustainable changes that promote optimal hormone balance and reduce systemic inflammation throughout the body.
Maintain a Healthy Weight
Excess body weight, particularly adipose tissue concentrated around the abdominal area, is a known contributor to increased estrogen production. Since estrogen fuels fibroid growth, maintaining a healthy weight is paramount. Numerous studies have consistently demonstrated that women with a higher Body Mass Index (BMI) face significantly elevated odds of developing fibroids. Gradual, sustained weight management achieved through a combination of balanced nutritional intake and consistent physical activity is often highly beneficial in this regard.
Prioritize Nutrient-Rich Foods
Dietary choices are powerful tools in supporting uterine health. Extensive research underscores the protective benefits of specific eating patterns:
- Abundant Fruits and Vegetables: Strive to consume a generous intake of fresh fruits and vegetables, aiming for at least four or more servings daily.
- Leafy Greens and Cruciferous Vegetables: Incorporate dark green leafy vegetables (e.g., spinach, kale) and cruciferous vegetables (e.g., broccoli, cauliflower, cabbage), which are rich in vitamins, minerals, and compounds that support detoxification and hormone metabolism.
- High-Fiber Whole Grains: Include diverse sources of dietary fiber from whole grains (e.g., oats, quinoa, brown rice). Fiber is essential for aiding the body in processing and excreting excess hormones, thereby contributing to hormonal balance.
- Vitamin D and Antioxidant-Rich Foods: Consider foods known to be associated with a lower fibroid risk, such as those naturally rich in Vitamin D (e.g., fatty fish, fortified dairy) and powerful antioxidants (e.g., green tea, berries), which combat inflammation and oxidative stress.
Stay Active Regularly
Consistent physical activity is not only vital for overall health but also serves as a critical component in managing weight and potentially reducing fibroid risk. A notable study, for instance, indicated that women engaging in higher levels of weekly exercise—such as brisk walking, dancing, or running—experienced a lower incidence of fibroids. The recommendation is to aim for at least 150 minutes of moderate-intensity aerobic activity per week. To help you get started, here’s an example of an approachable weekly activity plan:
- Monday, Wednesday, Friday: Dedicate 30 minutes to a brisk walk or a calming yoga session.
- Tuesday, Thursday: Focus on strength training or bodyweight exercises, incorporating movements like squats, lunges, or planks.
- Weekend: Engage in a longer, enjoyable activity such as hiking, cycling, or dancing.
- Daily Integration: If your job involves prolonged sitting, make an effort to stand up and stretch every hour to promote circulation and reduce sedentary time.
Managing uterine fibroids and supporting overall uterine health is an ongoing journey that often benefits from a holistic approach. By understanding the complex interplay of genetic, hormonal, and lifestyle factors, women are empowered to make informed choices. While some risk factors are beyond our control, actively embracing a nutrient-dense diet, maintaining a healthy weight, and engaging in regular physical activity can significantly contribute to hormone balance, reduce inflammation, and potentially mitigate fibroid development or alleviate symptoms. Always consult with a healthcare professional to discuss your specific condition and develop a personalized management plan.