Protecting Your Hands: Recognizing Early Signs of Hand Dermatitis and Essential Prevention Strategies
Our hands are constantly exposed to environmental stressors – from frequent washing and harsh cleaning agents to dry indoor air. This relentless exposure can gradually compromise the skin’s natural protective barrier. What often begins as minor dryness or a subtle patch of redness can escalate into persistent itching, painful cracks, and debilitating discomfort, hindering everyday activities like holding a mug or typing on a keyboard. Overlooking these initial indicators frequently results in more severe and widespread flare-ups, turning routine tasks into a struggle and potentially impacting sleep quality or professional productivity. The encouraging news is that adopting straightforward, scientifically-backed practices – such as consistent, targeted moisturizing and intelligent protective measures – can effectively safeguard your skin’s health and halt this progression before it worsens. Stay with us to uncover a surprising daily habit, supported by recent research, that could transform the comfort of your hands in a matter of weeks.
Understanding Hand Dermatitis: More Than Just Dry Skin
Hand dermatitis, often referred to as hand eczema, is an inflammatory skin condition predominantly affecting the hands and wrists. This common ailment impacts a significant portion of the global population, with prevalence rates reaching up to 10%. Data from reputable sources, including systematic reviews and studies published in journals like Contact Dermatitis, indicate a point prevalence of roughly 4-7% and a one-year prevalence approaching 10%. Research consistently shows a higher incidence among women (e.g., 10.6% compared to 5.2% in men) and individuals whose occupations involve frequent “wet work,” such as healthcare professionals, cleaners, or food service workers.
Globally, occupational skin diseases, with hand dermatitis accounting for a staggering 80-90% of cases, are recognized as the second most prevalent work-related illness. For instance, the U.S. Bureau of Labor Statistics reported 1.8 cases per 10,000 workers in 2020. Beyond its widespread occurrence, studies from publications such as The Lancet underscore its tendency to become chronic in up to two-thirds of affected individuals. This chronic nature can lead to persistent itching, discomfort, and a substantial reduction in quality of life, making even simple tasks like fastening buttons or engaging in confident handshakes challenging. Timely identification and intervention are crucial for effective management.
Unmasking the Triggers: What Causes Hand Dermatitis?
Hand dermatitis seldom develops without underlying factors. It typically arises from a complex interplay of elements that compromise the skin’s protective barrier, trigger allergic responses, or stem from individual predispositions such as genetics.
Irritant Contact Dermatitis: A Leading Cause
Among the various forms, irritant contact dermatitis stands out as the most common, particularly in occupational settings, accounting for 70-80% of cases according to reviews from institutions like the NIH. This non-allergic reaction occurs when the skin is repeatedly exposed to substances that strip away its natural oils, leading to cumulative damage. Common culprits include harsh soaps, potent detergents, and even excessive contact with water.
| Trigger Category | Typical Examples | Occupations at Higher Risk | Relevant Research Finding |
|---|---|---|---|
| Irritants | Strong soaps, frequent water exposure, alcohol-based sanitizers | Healthcare professionals, culinary staff, cleaning personnel | Responsible for approximately 80% of work-related cases (per PMC studies) |
| Allergens | Nickel, certain fragrances, natural rubber latex | Hair stylists, jewelry makers, manufacturing workers | Positive patch test results found in 19% of cases (as reported by The Lancet) |
| Atopic/Genetic Factors | Personal or family history of eczema, specific gene mutations (e.g., filaggrin) | Individuals in “wet work” environments with a family predisposition | Contributes to 22% of chronic hand dermatitis cases (NIH data) |
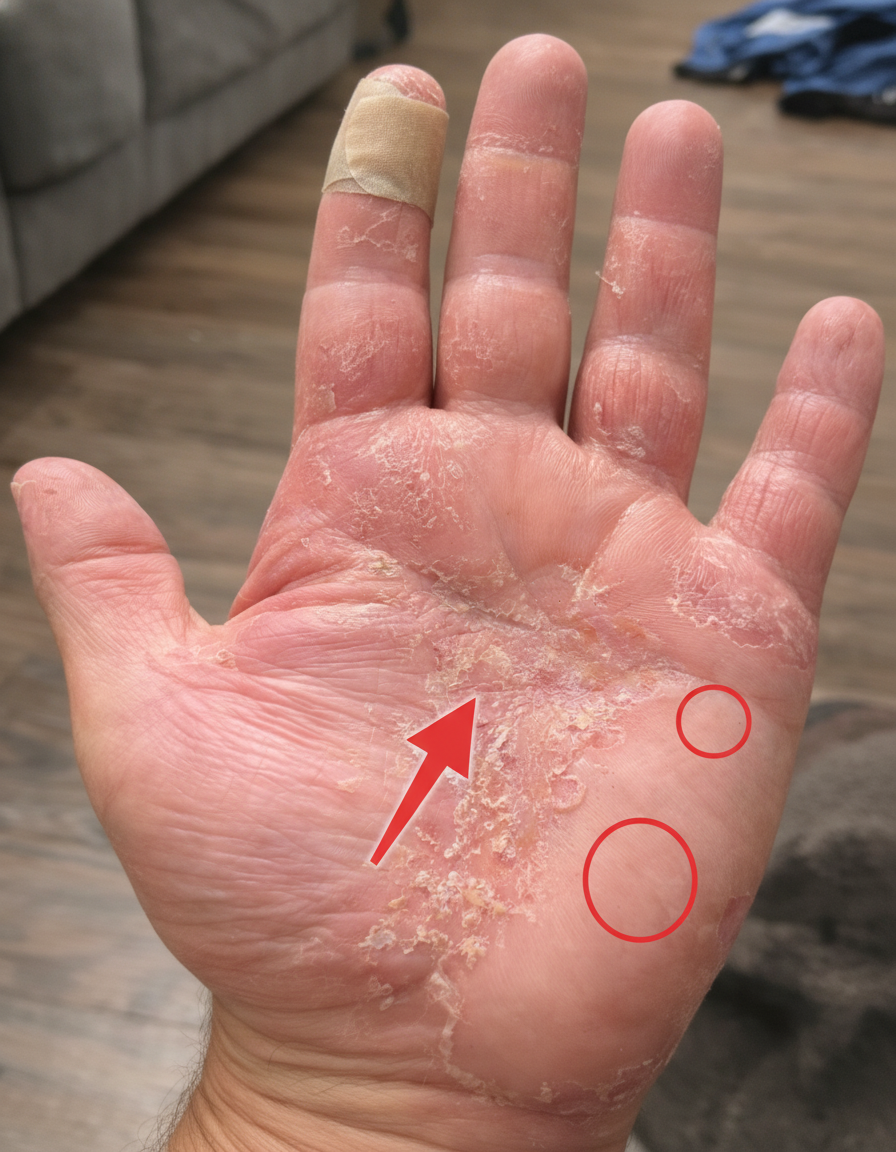
Recognizing the Red Flags: Early Symptoms of Hand Dermatitis
The indicators of hand dermatitis can range from subtle initial discomfort to severe, debilitating symptoms. While mild instances might be mistaken for ordinary dry skin, several distinct warning signs can help differentiate it:
- Persistent Itching: An irritating itch that doesn’t improve with standard moisturizing creams.
- Redness and Discomfort: Noticeable redness accompanied by a burning or stinging sensation across the palms, fingers, or backs of the hands.
- Dryness and Scaling: Patches of dry, flaking, or peeling skin, particularly prominent between the fingers.
- Painful Cracks: The appearance of painful cracks or fissures in the skin, which can bleed upon movement or contact.
- Small Blisters: Development of tiny, fluid-filled blisters (characteristic of dyshidrotic eczema), which may eventually lead to skin thickening.
During acute flare-ups, a review published in The Lancet highlights the presence of vesicles (small blisters) and edema (swelling). As the condition becomes chronic, the skin may undergo lichenification, appearing thick and rough. Notably, the hands are the primary site of initial manifestation in approximately 80% of dermatitis cases, according to resources like DermNetNZ.
Proactive Habits: Strengthening Your Skin Barrier and Preventing Flare-Ups
Effective prevention of hand dermatitis centers on supporting and fortifying the skin’s natural barrier. According to guidelines from organizations like Cochrane reviews and ESCD, emollients and barrier creams demonstrate protective benefits, though the extent of evidence can vary.
An Optimized Moisturizing Regimen
- Select Appropriate Products: Opt for rich, fragrance-free emollients, such as those formulated with ceramides or petrolatum. Research indicates these thicker preparations are more effective at repairing the skin’s stratum corneum lipids than lighter lotions.
- Apply Consistently: Make it a habit to moisturize after every hand wash and before bedtime. A randomized controlled trial (e.g., the Healthy Hands Project) has shown that structured skin care programs significantly reduce the risk of dermatitis among healthcare workers.
- Overnight Intensive Care: For an enhanced effect, apply a generous layer of moisturizer and wear cotton gloves overnight. Pilot studies suggest that fabric gloves can boost skin hydration and lessen the severity of dermatitis symptoms (improving OHSI scores).
Smart Practices for Hand Washing and Protection
- Utilize Protective Gloves: When performing wet tasks, wear cotton liners beneath vinyl or nitrile gloves. To prevent skin maceration, avoid prolonged use of completely occlusive gloves. Some trials suggest semi-permeable options (like Sympatex) may facilitate recovery more effectively than cotton alone.
- Gentle Hand Cleansing: Always use pH-neutral, soap-free cleansers. Ensure thorough rinsing and gently pat your hands dry with a soft towel, rather than rubbing vigorously. Opt for alcohol-based hand gels when hands are not visibly soiled, as they are generally less irritating than repeated cycles of soap and water.
- Steer Clear of Environmental Extremes: Minimize exposure to very hot or very cold water, and reduce the duration of hand sanitization when possible.